Disc Anatomy
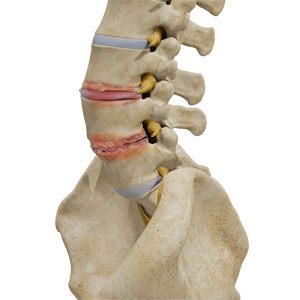
The intervertebral discs are soft cushions located between the bones of the spine (vertebrae). Each disc is composed of two main parts:
- Annulus fibrosus – a strong outer ring of fibrous tissue
- Nucleus pulposus – a soft, gel-like center
The discs are anchored between adjacent vertebral bodies by cartilaginous endplates. These discs allow the spine to move smoothly while helping distribute forces during everyday activities such as walking, bending, and lifting.
Intervertebral discs function as shock absorbers, protecting the spine from excessive mechanical stress.
What is Degenerative Disc Disease?
Degenerative Disc Disease (DDD) refers to the gradual breakdown or deterioration of the intervertebral discs between the vertebrae. Despite the name, it is not truly a disease, but rather a condition related to aging and normal wear of the spine.
Over time, discs lose water content and elasticity, making them less able to absorb stress. As discs degenerate, they may lose height, develop small tears, or become less flexible.
Degenerative changes in spinal discs are extremely common. Studies show that:
- More than 80–90% of adults over age 60 have some degree of disc degeneration on imaging.
- Disc degeneration can begin as early as the third decade of life.
- Many individuals have degenerative changes on MRI without experiencing symptoms.
DDD most commonly affects the cervical spine (neck) and lumbar spine (lower back).
Prevalence and Healthcare Impact
Low back pain related to degenerative disc disease is one of the most common health problems worldwide.
- Low back pain is the leading cause of disability globally.
- Up to 80% of people experience significant back pain at some point in their lives.
- Degenerative spine conditions are among the most common reasons adults seek medical care.
- In the United States, back and neck pain account for over $100 billion annually in healthcare costs, lost productivity, and disability.
Because of its prevalence and impact on mobility, degenerative disc disease represents a major public health issue.
Causes of Degenerative Disc Disease
As the body ages, the rate at which damaged cells are replaced gradually decreases. This can lead to structural changes in the intervertebral discs.
Common contributing factors include:
- Natural aging of the spine
- Repetitive strain or heavy lifting
- Injury or trauma
- Poor posture or body mechanics
- Smoking
- Genetic predisposition
Degenerative changes in the discs may result in:
- Loss of disc height
- Reduced spinal flexibility
- Small tears in the annulus fibrosus
- Formation of bone spurs (osteophytes)
These changes may also contribute to other spinal conditions such as:
- Herniated discs
- Spinal stenosis
- Facet joint arthritis (spondylosis)
Symptoms of Degenerative Disc Disease
Not all individuals with degenerative disc disease develop symptoms. However, when symptoms occur, they may include:
- Chronic neck or low back pain
- Pain that worsens with bending, lifting, or twisting
- Stiffness and reduced spinal mobility
- Pain that improves with rest or position changes
- Pain radiating into the arms or legs if nerves are compressed
- Numbness, tingling, or weakness in the extremities
Degeneration in the lumbar spine often causes lower back pain and sometimes leg pain. Degeneration in the cervical spine may cause neck pain and symptoms that radiate into the shoulders or arms.
When Patients Seek Medical Care
Many people with degenerative disc disease initially manage symptoms on their own. Patients commonly seek medical evaluation when they experience:
- Persistent back or neck pain lasting several weeks
- Pain that interferes with daily activities or sleep
- Pain radiating into the arms or legs
- Numbness, tingling, or weakness
- Difficulty walking, standing, or performing normal activities
Evaluation by a spine specialist can help determine the cause of symptoms and identify appropriate treatment options.
Diagnosis of Degenerative Disc Disease
Diagnosis typically involves a detailed medical history and physical examination.
During the examination, the physician may evaluate:
- Spinal flexibility and range of motion
- Areas of tenderness
- Muscle strength and reflexes
- Signs of nerve irritation
Imaging studies may be used to confirm the diagnosis.
X-rays
X-rays may show narrowing of the disc space, indicating disc thinning or collapse. Bone spurs around the vertebrae may also be visible.
MRI or CT Scan
An MRI scan provides detailed images of the discs, nerves, and soft tissues and can identify disc degeneration, disc herniation, and nerve compression.
A CT scan may be used to evaluate the bony structures of the spine and the space available for nerve roots.
Treatment of Degenerative Disc Disease
Treatment depends on the severity of symptoms and the presence of nerve compression.
Non-Surgical Treatment
Most patients improve with conservative treatment options such as:
- Anti-inflammatory medications
- Activity modification
- Physical therapy
- Core strengthening exercises
- Heat or ice therapy
- Epidural steroid injections in selected cases
These treatments aim to reduce inflammation, improve spinal stability, and restore function.
Surgical Treatment
Surgery is typically considered only when non-surgical treatments fail to relieve symptoms or when there is significant nerve compression causing pain, numbness, or weakness.
Possible surgical treatments include:
- Spinal decompression: Removal of bone or tissue compressing the nerves.
- Discectomy: Removal of the damaged portion of a disc.
- Spinal fusion: Stabilization of the spine by joining two adjacent vertebrae.
- Artificial disc replacement: In select patients, disc replacement may be performed to preserve motion in the spine.
Summary
Degenerative disc disease is a common age-related condition affecting the spinal discs. Although many people have disc degeneration without symptoms, others may experience back or neck pain and nerve-related symptoms.
Early evaluation and appropriate treatment can help relieve pain, restore mobility, and improve quality of life.











