What Is Pseudarthrosis?
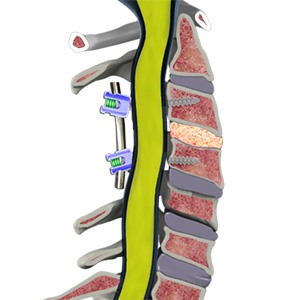
Pseudarthrosis, also known as spinal nonunion, occurs when bones that were intended to fuse together after spinal fusion surgery fail to heal into a solid bone.
The term “pseudarthrosis” literally means “false joint.” Instead of forming a solid fusion, the bones remain separated and may continue to move slightly. This movement can lead to persistent pain, spinal instability, or hardware complications.
Spinal fusion surgery is commonly performed to stabilize the spine for conditions such as degenerative disc disease, spinal deformity, spinal instability, or fractures. While most spinal fusions heal successfully, in some cases the bone does not fully fuse.
How Common Is Pseudarthrosis?
The likelihood of pseudarthrosis depends on several factors including the number of spinal levels fused and the patient’s overall health.
Studies suggest:
- Fusion rates for many procedures exceed 90%, particularly in single-level surgeries.
- The risk of nonunion may increase in multilevel fusions, revision surgeries, or patients with certain medical risk factors.
Advances in surgical techniques, bone graft materials, and biologic agents have significantly improved fusion success rates.
Causes of Pseudarthrosis
Spinal fusion requires bone healing between two or more vertebrae. When this healing process is disrupted, fusion may fail to occur.
Common causes include:
- Inadequate Bone Healing: Bone graft placed during surgery may not fully incorporate into the surrounding bone.
- Excessive Motion: Movement at the fusion site can interfere with bone healing.
- Poor Bone Quality: Conditions such as osteoporosis can reduce the ability of bone to heal properly.
- Infection: Infection following spinal surgery can disrupt the bone healing process.
- Hardware Failure: In rare cases, screws or rods used to stabilize the spine may loosen or break if fusion does not occur.
Risk Factors:
Several factors can increase the risk of pseudarthrosis.
Common risk factors include:
- Smoking or nicotine use, which significantly impairs bone healing
- Diabetes
- Osteoporosis
- Obesity
- Malnutrition
- Chronic steroid use
- Multilevel spinal fusion surgery
- Previous spinal surgery (revision procedures)
Smoking is considered one of the most significant risk factors for spinal nonunion.
Symptoms of Pseudarthrosis
Some patients with pseudarthrosis may have few or no symptoms, while others develop persistent pain after surgery.
Common symptoms include:
- Ongoing back or neck pain after spinal fusion surgery
- Pain that initially improved after surgery but later returned
- Mechanical pain with movement or activity
- Persistent nerve symptoms such as leg or arm pain
- Feeling of spinal instability
In some cases, hardware used during the fusion procedure may loosen or break, which can cause additional pain.
Diagnosis
Diagnosis of pseudarthrosis begins with a clinical evaluation and imaging studies.
Your physician will review:
- Surgical history
- Symptoms and pain patterns
- Physical examination findings
Imaging studies may include:
- X-rays: Standing X-rays can show whether the bones have fused and may detect hardware complications.
- CT Scan: A CT scan is often the most accurate imaging test for evaluating bone healing and identifying pseudarthrosis.
- MRI: MRI scans may help evaluate nerve compression, inflammation, or other soft tissue changes.
These imaging studies help determine whether the fusion has healed properly.
Treatment
Treatment depends on the severity of symptoms and whether the spine remains stable.
Non-Surgical Treatment
In some cases, pseudarthrosis may be managed without additional surgery.
Non-surgical treatment options may include:
- Activity modification
- Physical therapy
- Pain management treatments
- Bracing in selected cases
If symptoms are mild and the spine remains stable, observation may be appropriate.
Bone Growth Stimulators
In certain cases, physicians may recommend the use of bone growth stimulators to help promote fusion.
Bone growth stimulators are devices that deliver electrical or electromagnetic signals to the spine that can stimulate bone healing. These signals activate cellular pathways involved in bone formation and may help improve the likelihood of successful fusion.
These devices are typically worn externally over the spine for several hours each day during the healing process.
Bone stimulators are most commonly used in patients who have a higher risk of nonunion, such as:
- Patients undergoing multilevel spinal fusion
- Revision fusion surgery
- Patients with osteoporosis or poor bone quality
- Smokers or former smokers
- Patients with early evidence of delayed fusion
While bone growth stimulators do not guarantee fusion, studies suggest they may improve healing in selected high-risk patients and are often used as an adjunct to other treatments.
Surgical Treatment
Surgery may be recommended when:
- Persistent pain significantly affects quality of life
- Spinal instability develops
- Hardware failure occurs
- Nerve compression is present
Revision surgery for pseudarthrosis focuses on achieving successful fusion and restoring spinal stability.
Common surgical approaches include:
- Revision Spinal Fusion: The surgeon may perform a repeat fusion procedure using additional bone graft material and new instrumentation such as screws and rods.
- Bone Grafting: Bone graft from the patient, a donor source, or synthetic materials may be used to promote bone healing.
- Biologic Fusion Enhancers: In some cases, biologic agents such as bone morphogenetic proteins (BMP) may be used to stimulate bone growth and improve fusion rates.
The specific surgical approach depends on the location of the fusion, the number of levels involved, and the patient’s overall health.
Summary
Pseudarthrosis, or spinal nonunion, occurs when bones fail to fuse successfully following spinal fusion surgery. While most spinal fusions heal properly, certain factors such as smoking, poor bone quality, and multilevel surgery can increase the risk of nonunion. Symptoms may include persistent pain, spinal instability, or hardware complications. Diagnosis typically involves imaging studies such as CT scans to evaluate bone healing. Treatment may include conservative management, bone growth stimulation, or revision spinal fusion surgery to restore spinal stability and promote proper bone healing.











