What Is the Sciatic Nerve?
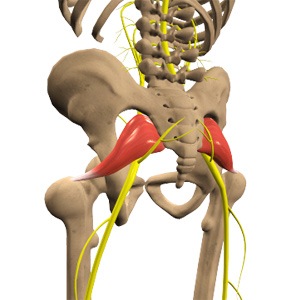
The sciatic nerve is the largest nerve in the body. It begins in the lower spine and travels through the buttocks and down the back of each leg to the foot.
This nerve plays a major role in controlling movement and sensation in the legs and feet. When the nerve becomes irritated or compressed, it can cause pain and neurological symptoms that travel along its path.
What Is Sciatica?
Sciatica refers to pain caused by irritation or compression of the sciatic nerve. It is important to understand that sciatica is a symptom rather than a diagnosis, meaning that it is usually caused by an underlying spine condition.
Sciatica may be:
- Acute, lasting a few days to several weeks
- Chronic, lasting longer than three months
In many cases, symptoms improve with time and conservative treatment.
Causes of Sciatica
Several conditions can irritate or compress the sciatic nerve, including:
- Herniated disc
- Lumbar spinal stenosis
- Degenerative disc disease
- Spondylolisthesis
- Piriformis syndrome
- Spinal tumors or trauma
Among these, lumbar disc herniation is the most common cause of sciatica, particularly in younger and middle-aged adults.
Risk Factors
Certain factors may increase the likelihood of developing sciatica:
- Increasing age
- Sedentary lifestyle
- Repetitive physical strain or occupational lifting
- Smoking
- Diabetes
- Poor physical conditioning
Jobs that involve prolonged sitting, heavy lifting, or repetitive bending may also increase the risk.
Symptoms of Sciatica
The hallmark symptom of sciatica is pain radiating down the leg, but symptoms can vary depending on the degree of nerve irritation.
Common symptoms include:
- Pain in the buttock or leg
- Sharp, shooting pain down the leg
- Numbness or tingling in the leg or foot
- Weakness in the leg or foot
- Pain that worsens when sitting or bending
Pain may also increase with coughing, sneezing, straining, or prolonged sitting.
Diagnosis
Diagnosis begins with a review of your medical history and symptoms along with a physical examination.
Your physician may evaluate:
- Muscle strength
- Reflexes
- Areas of numbness or tingling
- Leg raise testing to reproduce symptoms
Imaging studies may be performed to identify the underlying cause of nerve compression.
These may include:
- MRI scans
- CT scans
- X-rays
Additional tests such as electromyography (EMG) or nerve conduction studies may be used to evaluate nerve function.
Treatment
Most cases of sciatica improve with non-surgical treatment.
Non-Surgical Treatment
Common conservative treatments include:
- Physical therapy and stretching exercises
- Anti-inflammatory medications
- Ice or heat therapy
- Epidural steroid injections
- Activity modification
Outcomes of Conservative Care
The majority of patients experience improvement with conservative treatment. Studies show that approximately 70–90% of patients with sciatica improve without surgery within several weeks to a few months.
However, some patients may experience recurrent episodes of sciatica, particularly when degenerative spine conditions or disc herniations persist.
Surgical Treatment
Surgery may be recommended when:
- Pain persists despite several weeks to months of conservative treatment
- Significant nerve compression causes weakness or neurological deficits
- Symptoms severely limit daily activities
The most common surgical treatment for sciatica caused by a herniated disc is lumbar microdiscectomy, which removes the portion of the disc compressing the nerve.
Other procedures may be recommended depending on the underlying cause of nerve compression, such as decompression surgery for spinal stenosis.
Summary
Sciatica is a common condition caused by irritation or compression of the sciatic nerve, resulting in pain that radiates from the lower back into the buttock and leg. In most cases, symptoms improve with conservative treatment such as physical therapy, medications, and activity modification. However, persistent or recurrent symptoms may require surgical treatment to relieve pressure on the affected nerve and restore normal function.











