What Are Spinal Infections?
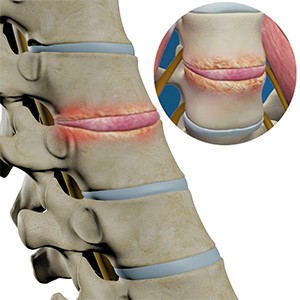
A spinal infection occurs when bacteria or other microorganisms infect the bones, discs, or surrounding tissues of the spine. Although relatively uncommon, spinal infections can be serious because they may damage spinal structures or compress the spinal cord and nerves.
Spinal infections most commonly affect the vertebrae (spinal bones) or the intervertebral discs, but they may also involve the epidural space surrounding the spinal cord.
Early diagnosis and treatment are important to prevent complications such as bone destruction, spinal instability, or neurological injury.
Types of Spinal Infections
Several different types of infections can affect the spine.
Discitis and Osteodiscitis
Discitis refers to infection of the intervertebral disc, the cushioning structure between two vertebrae. Because the disc and adjacent vertebral bones share blood supply, infections often involve both structures.
When both the disc and surrounding vertebrae are infected, the condition is called osteodiscitis.
These infections most commonly occur in the lumbar spine (lower back) but may also occur in the thoracic or cervical spine.
Vertebral Osteomyelitis
Osteomyelitis refers to infection of the bone itself. When this occurs in the spine, the vertebral bodies become infected and may gradually weaken or collapse.
Vertebral osteomyelitis is the most common type of spinal infection in adults.
The infection often spreads to the spine through the bloodstream from another part of the body.
Spinal Epidural Abscess
A spinal epidural abscess is a collection of infected material (pus) that forms in the epidural space surrounding the spinal cord.
As the abscess grows, it may compress the spinal cord or nerve roots, which can lead to serious neurological complications if not treated promptly.
Epidural abscesses are considered a medical emergency because rapid treatment may be required to prevent permanent neurological damage.
Causes of Spinal Infections
Spinal infections are most commonly caused by bacteria that spread through the bloodstream to the spine.
Common sources of infection include:
- Skin infections
- Urinary tract infections
- Lung infections
- Intravenous drug use
- Recent surgery or invasive medical procedures
- Bloodstream infections
The most common organism responsible for spinal infections is Staphylococcus aureus, though other bacteria, fungi, or tuberculosis can also cause spinal infections.
Risk Factors
Certain conditions may increase the risk of developing spinal infections.
Risk factors include:
- Diabetes
- Weakened immune system
- Cancer or chemotherapy treatment
- Intravenous drug use
- Chronic kidney disease
- Advanced age
- Recent spinal surgery or injections
Patients with these conditions may be more susceptible to infection spreading to the spine.
Symptoms of Spinal Infections
Symptoms may develop gradually and can sometimes be difficult to recognize early.
Common symptoms include:
- Persistent back or neck pain
- Fever or chills
- Fatigue
- Muscle spasms
- Pain that worsens with movement
As the infection progresses, patients may develop neurological symptoms such as:
- Numbness or tingling
- Weakness in the arms or legs
- Difficulty walking
- Loss of bladder or bowel control
When neurological symptoms occur, urgent medical evaluation is necessary.
Diagnosis
Diagnosis begins with a detailed medical history and physical examination.
Your physician may evaluate:
- Location and severity of pain
- Neurological function
- Signs of systemic infection
Laboratory tests may include:
- Blood tests to detect inflammation or infection
- Blood cultures to identify bacteria in the bloodstream
Imaging studies are critical for diagnosing spinal infections.
Common imaging tests include:
- MRI scans, which are the most sensitive test for detecting spinal infection
- CT scans, which help evaluate bone destruction
- X-rays, which may show structural changes in later stages
In some cases, a needle biopsy may be performed to identify the specific organism causing the infection.
Treatment
Treatment of spinal infections depends on the severity of the infection and whether the spinal cord or nerves are affected.
Non-Surgical Treatment
Many spinal infections can be treated successfully with antibiotic therapy.
Treatment typically includes:
- Intravenous antibiotics for several weeks
- Pain management medications
- Bracing to stabilize the spine during healing
- Monitoring with repeat imaging and laboratory tests
Antibiotic treatment may continue for 6 to 12 weeks or longer, depending on the type of infection.
Surgical Treatment
Surgery may be required if:
- The infection causes spinal cord or nerve compression
- There is spinal instability due to bone destruction
- The infection does not respond to antibiotics
- Large abscesses develop around the spinal cord
Surgical treatment may involve:
- Abscess Drainage: Removing infected fluid to relieve pressure on the spinal cord.
- Spinal Decompression: Removing infected bone or tissue that is compressing nerves.
- Spinal Stabilization: If the infection weakens the spine, screws, rods, and spinal fusion may be used to stabilize the spinal column.
These procedures help eliminate infection while protecting neurological function and restoring spinal stability.
Summary
Spinal infections are uncommon but potentially serious conditions that affect the bones, discs, or surrounding tissues of the spine. Conditions such as osteomyelitis, osteodiscitis, and spinal epidural abscess may cause persistent back pain, fever, and neurological symptoms if the spinal cord or nerves become compressed. Early diagnosis using imaging and laboratory tests is critical. Treatment typically involves prolonged antibiotic therapy, while surgery may be necessary in cases of spinal instability, abscess formation, or neurological compression.











