What Are Spinal Fractures?
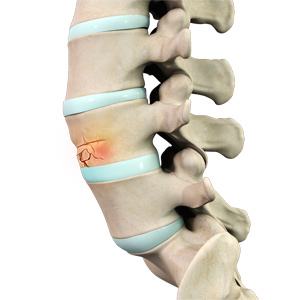
A spinal fracture occurs when one or more of the bones of the spine, called vertebrae, break or collapse. These injuries may occur as a result of trauma, osteoporosis, cancer, or other conditions that weaken the bones of the spine.
The severity of spinal fractures can vary widely. Some fractures are stable and cause mild pain, while others may lead to spinal instability or compression of the spinal cord or nerves.
Spinal fractures most commonly occur in the thoracic spine (mid-back) and lumbar spine (lower back).
Types of Spinal Fractures
Several types of spinal fractures can occur depending on the mechanism of injury and the part of the vertebra involved.
Compression Fractures
Compression fractures are the most common type of spinal fracture. They occur when the front portion of a vertebral body collapses or becomes compressed.
This type of fracture is most commonly associated with osteoporosis, a condition in which bones become weaker and more fragile.
Compression fractures can cause the vertebra to become wedge-shaped, which may lead to progressive spinal curvature or kyphosis if multiple fractures occur.
Burst Fractures
A burst fracture occurs when a vertebra breaks in multiple directions, often due to high-energy trauma such as motor vehicle accidents or significant falls.
Unlike compression fractures, burst fractures may push bone fragments into the spinal canal and can potentially compress the spinal cord or spinal nerves.
Flexion-Distraction Fractures
These fractures occur when the spine is forced to bend forward suddenly, often during high-impact trauma such as automobile accidents.
This injury may involve both bone and ligament damage and can lead to spinal instability.
Fracture-Dislocations
Fracture-dislocations are severe injuries involving both a spinal fracture and displacement of the vertebrae. These injuries typically result from major trauma and often require urgent medical attention.
Causes of Spinal Fractures
Spinal fractures may occur for several reasons.
Common causes include:
- Osteoporosis: Osteoporosis weakens the bones and is the most common cause of compression fractures in older adults. Even minor falls or routine activities may lead to fractures in weakened bones.
- Trauma: High-energy injuries such as motor vehicle accidents, sports injuries, or falls from height can cause spinal fractures.
- Tumors or Cancer: Cancer that spreads to the spine can weaken the vertebrae and make them more susceptible to fracture.
- Infections: Certain infections affecting the spine may weaken bone structure and increase fracture risk.
Symptoms of Spinal Fractures
Symptoms depend on the severity and location of the fracture.
Common symptoms include:
- Sudden back pain
- Pain that worsens with standing or walking
- Limited spinal mobility
- Muscle spasms
- Height loss
When multiple compression fractures occur, patients may develop a forward stooping posture due to progressive spinal curvature.
If the spinal cord or nerves are compressed, symptoms may include:
- Numbness or tingling
- Weakness in the arms or legs
- Difficulty walking
- Loss of bowel or bladder control in severe cases
Diagnosis
Diagnosis begins with a medical history and physical examination.
Your physician will evaluate:
- Location of pain and tenderness
- Spinal alignment and posture
- Neurological function
Imaging studies are essential to confirm the diagnosis and determine fracture stability.
Common diagnostic tests include:
- X-rays, which can identify vertebral collapse or deformity
- MRI scans, which help determine whether the fracture is new and evaluate nerve compression
- CT scans, which provide detailed images of bone structures
These tests help determine whether the fracture is stable or unstable, which guides treatment decisions.
Treatment
Treatment depends on the type of fracture, its stability, and whether the spinal cord or nerves are involved.
Non-Surgical Treatment
Many spinal fractures, particularly compression fractures, can be treated without surgery.
Non-surgical treatments may include:
- Pain medications
- Activity modification
- Bracing to stabilize the spine during healing
- Physical therapy to strengthen the back and core muscles
- Treatment of underlying osteoporosis
Most stable compression fractures gradually improve over several weeks to months.
Minimally Invasive Fracture Treatment
For painful compression fractures that do not improve with conservative treatment, minimally invasive procedures may be considered.
Vertebroplasty
Vertebroplasty involves injecting medical bone cement into the fractured vertebra to stabilize the bone and reduce pain.
Kyphoplasty
Kyphoplasty is similar to vertebroplasty but involves inserting a small balloon into the vertebra to help restore height before cement is placed.
These procedures can help stabilize the fracture and relieve pain in selected patients.
Surgical Treatment
Surgery may be necessary when:
- The fracture causes spinal instability
- Bone fragments compress the spinal cord or nerves
- The spine becomes significantly misaligned
- Severe pain persists despite conservative treatment
Surgical treatment may include decompression of the spinal cord or nerves, along with spinal stabilization using screws, rods, and fusion techniques.
In cases where the vertebral body is severely damaged, procedures such as corpectomy may be performed to remove the fractured bone and reconstruct the spine.
Summary
Spinal fractures occur when one or more vertebrae in the spine break or collapse. These fractures may result from osteoporosis, trauma, cancer, or other conditions that weaken the bones. Compression fractures are the most common type and often occur in individuals with osteoporosis. Symptoms may include sudden back pain, reduced mobility, and changes in posture. Treatment depends on the severity of the fracture and may range from bracing and conservative care to minimally invasive procedures or surgical stabilization in more severe cases.











